
In 2019, CMS placed new requirements on hospitals in an effort to provide consumers with easily accessible information on health care costs. How will these requirements impact your hospital if they take effect in 2021?
“We also continue to believe that price transparency will lead to lower costs for consumers and better quality of care.” CMS, final price transparency rule (CMS 1717-F2)
Better quality. Lower costs. Those are ongoing, cross-cutting agency goals for the Centers for Medicare and Medicaid (CMS) that are interwoven into the agency’s policies impacting reimbursements, new payment models, care delivery, and hospital price transparency.
On December 4, 2019, four hospital associations and several hospitals filed suit to block the CMS hospital price transparency policy. They cited the agency’s lack of authority, compelled speech, and trade secret law as rationales.
You might remember that CMS dove into price transparency more intently in 2019 with the requirement that all hospitals post their chargemasters online in a machine-readable format. That requirement is still in effect. However, on November 15, 2019, CMS finalized a far-reaching expansion of its original policy. If allowed to stand, these new requirements will take effect January 1, 2021.
Key hospital price transparency definitions
There are several key definitions to keep in mind with the new requirements. First, CMS broadly defines hospitals based on state or local licensing, irrespective of Medicare or federal status. Second, CMS broadly defines “items and services” to include all items and services, as well as service packages in the inpatient or outpatient setting. Finally, CMS defines five types of “standard charges” that all hospitals are required to post:
- Gross charge: the charge for an individual item or service that is reflected on a hospital’s chargemaster, absent any discounts
- Payer-specific negotiated charge: the charge that a hospital has negotiated with a third-party payer for an item or service
- Discounted cash price: the charge that applies to an individual who pays cash, or cash equivalent, for a hospital item or service
- De-identified minimum negotiated charge: the lowest charge that a hospital has negotiated with all third-party payers for an item or service
- De-identified maximum negotiated charge: the highest charge that a hospital has negotiated with all third-party payers for an item or service
Public posting requirements
Under CMS’s final rule (1717-F2), hospitals are required to post standard charges in two ways: for all hospital items and services, and for 300 “shoppable” services.
In the first requirement, CMS mandates posting the chargemaster, including all five of the standard charges, along with additional information such as CPT or HCPCS codes (among others). The information must be posted in a machine-readable format and easy to find on the website.
What Can You Do?
- Dig into the price transparency rule and begin taking steps to comply.
- Find exemplars, seek out best practices, and learn lessons from organizations who are already along the price transparency path.
- Review your financial/revenue cycle functions and price estimator tools, especially from the patient perspective.
With respect to the second requirement —to post “shoppable services” — CMS defines “shoppable services” as something that can be scheduled by a health care consumer in advance. CMS mandates 70 of the services, with the hospital allowed to determine the other 230. The 70 mandated services fall under the following categories: Evaluation and Management Services, Laboratory and Pathology Services, Radiology Services, and Medicine and Surgery Services.
In addition, CMS requires plain language descriptions of the shoppable services, ancillaries that would go along with those services, and the locations where those services are offered. The good news? CMS will deem hospital price estimator tools that meet certain criteria as meeting this second requirement.
Failure to comply
While the original 2019 regulation did not include penalties for failure to post a hospital chargemaster, CMS finalized enforcement mechanisms for the 2021 requirement. Generally, CMS indicates it can:
- Issue a written warning notice to hospitals that fail to make public their standard charges or fail to do so in the manner prescribed in the new regulation
- Request a corrective action plan (CAP) in the case of serious violations
- Impose a civil monetary penalty (CMP) and publicize the penalty on a CMS website if a hospital fails to submit a CAP or doesn’t comply with the terms of a CAP
Enforcement actions do not necessarily have to follow the sequence described above. CMS may initiate an audit of a hospital’s website or review third-party complaints that have been submitted, and the fine is $300 per day for noncompliance. It’s also important to note that there is an appeals process for the CMP.
Why price transparency now?
Health expenditures continue to increase. According to the Office of the Actuary for CMS, national health expenditures are projected to increase an average of 5.5% each year from 2018 to 2027, ultimately totaling $6 trillion by 2027. While insurance coverage is expected to remain stable, out-of-pocket costs — whether those are co-pays, deductibles, or premiums — continue to grow as well. In 2018, the latter accounted for $375.6 billion (which equates to 10%) of all health care expenditures. The ongoing cost dynamic places a strain on federal, state, employer, and consumer budgets. It is why value-based payment models are attracting more attention across all payers, and why regulators are looking at health care prices.
There are other dynamics at play as well. There has been an uptick in health care mergers, both horizontal and vertical. The Department of Justice and Federal Trade Commission released new draft guidance on vertical mergers. All of the activity gives rise to questions on whether hospital mergers and acquisitions play a positive or negative role in addressing costs. There are those who believe mergers lead to reduced costs and better quality. Others believe the opposite: that deals are only for gaining market share — and hence, negotiating leverage — with no savings passed on to payers or consumers. Even worse, costs go up and patient experience outcomes decline.
Concurrently, new entrants are coming into the market, and some have pre-set prices. In direct primary care models, a set fee is paid over the year for all primary care visits. Another example is Walmart’s new primary care clinic where, for between $20 and $60, an individual can receive a medical, dental, optometry, or counseling visit, and no insurance is required. In these situations, the consumer can easily see and understand their costs. Coupled with technological capabilities that facilitate how consumers engage with the health care system, now consumers can compare and shop for what is currently out there. Granted, these options are not broad-based yet, but they are growing.
With this in mind, the federal government knows it has levers it can use, as the largest health care payer, to drive transparency forward. For example, CMS launched a consumer look-up tool to compare hospital outpatient department costs to those at an ambulatory surgical center.
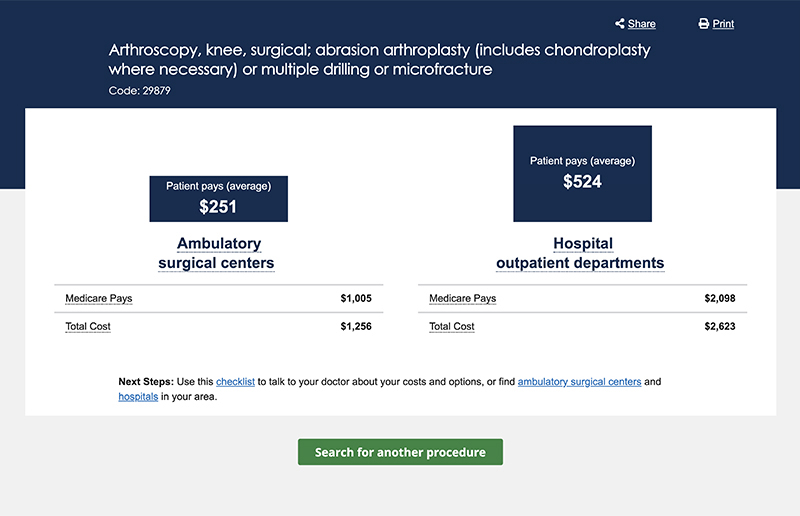
The newest price transparency regulation builds on these dynamics. It is an aggressive play, but it is in line with the agency’s stated and ongoing commitment to advancing “value.” From the MyHealthEData initiative to encouraging the use of application programming interfaces (APIs) to its proposed interoperability rule, the agency most definitely views consumerism, patient access to their own health data, and prices as key aspects to advance that goal.
How CLA can help
Whether the court ultimately rules against the price transparency rule is still to be determined, but there are lessons to be learned. Price matters. Consumers matter. Quality and outcomes matter. Even though the health care financing system is complex, helping patients navigate and understand it in a meaningful way is important.
If you need assistance understanding new regulations and the potential for future congressional activity — as well as market analysis, revenue cycle review, and future-oriented insights — CLA is always here to help.
